

A breakthrough non-surgical solution for osteoarthritis that relieves pain, protects cartilage, and restores movement — all with a single injection.
This is presently the gold standard , non-surgical treatment for Osteoarthritis. With just one injection, you can have 70% improvement from joint pain and stiffness for up to 2-3 years.1,2 Not only this, but you can also improve joint function and possibly slow the destruction of cartilage.3,4
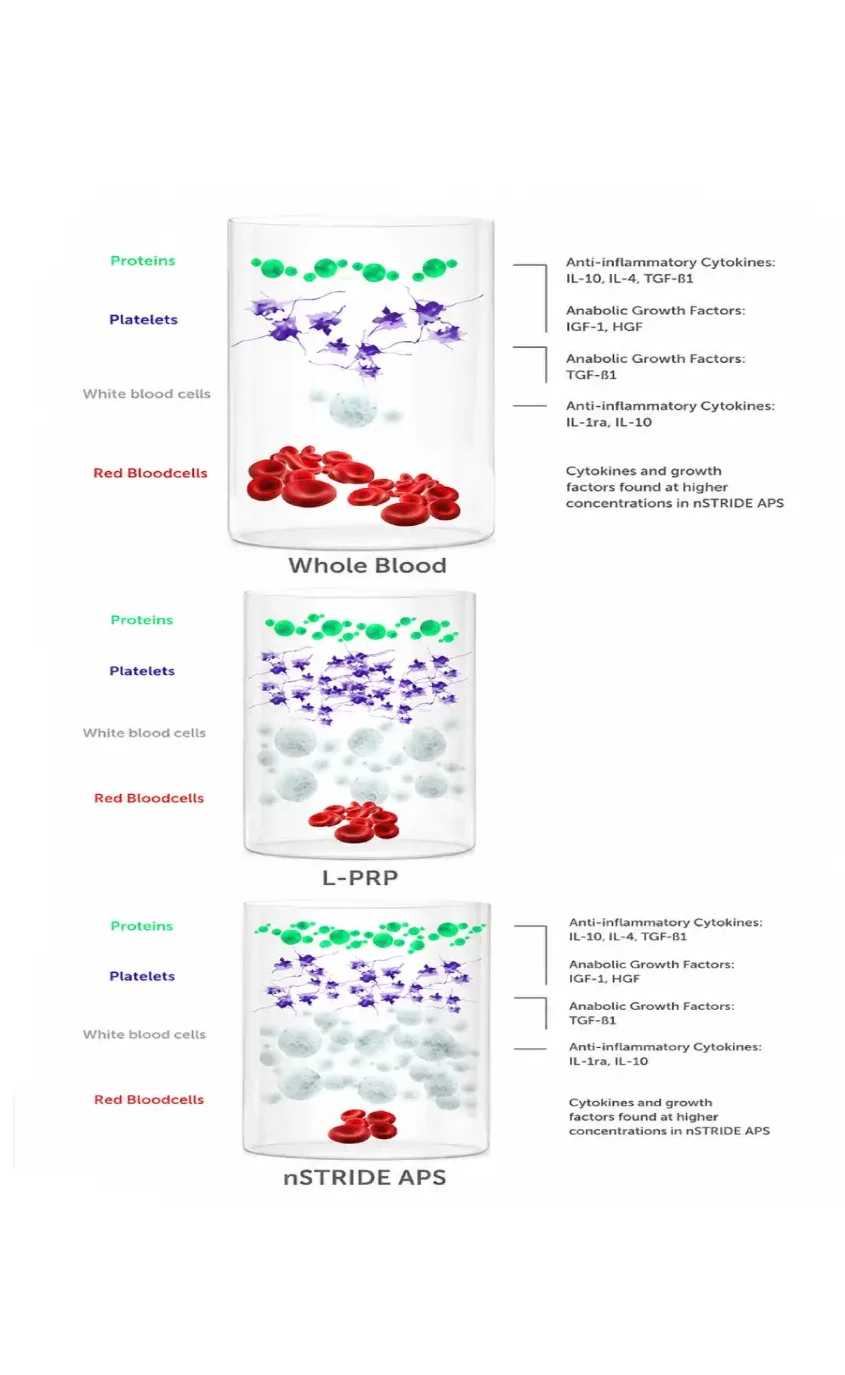
The process is similar to a PRP injection, as a sample of blood is first taken from the arm, and the processed. It’s different in the sense that the sample is then process a second time, specifically to isolate and increase the number of anti-inflammatory proteins. Compared to normal blood, the solution at the end may have up to 1000 times the normal concentration of good proteins to decrease pain and protect cartilage.
Presently, this technique is approved by Health Canada to treat Knee Osteoarthritis. Research is ongoing for other parts of the body. Given its safety profile, this can also be administered to other joints, tendons, and ligaments, with discussion from your physician. It does not work for everybody. Please speak with your physician if this is the right treatment for you.
Provides significant reduction in joint pain and stiffness for up to 2–3 years after a single treatment.
Concentrated anti-inflammatory proteins help slow cartilage breakdown and protect joint health.
Concentrated anti-inflammatory proteins help slow cartilage breakdown and protect joint health.
Protein Solution Injection is highly biocompatible, but some mild reactions may occur.
Please see our fees and financing for more information.
REHABILITATION SERVICES
Unit 303: Physiotherapy, Massage Therapy,
Chiropractic, Custom Bracing, DEXA Body Scans
Mon, Wed, Fri : 8 am to 7 pm
Tues, Thurs : 8 am to 5 pm
Sat to Sun : Closed
MEDICAL SERVICES
Unit 303: Rheumatology, Neurology, Psychiatry, Lifestyle Medicine
Unit 304: Physical Medicine, NCS/EMG, US-Guided Injections
Mon to Fri : 8 am to 5 pm
Sat to Sun : Closed
(Hours and availability may vary)